Thus, a large population must be evaluated to assess the role of Rh blood type in identifying women at risk of developing pregnancy-related complications. Moreover, the Rh-negative population is extremely small. However, data about whether maternal Rh blood type alone, without consideration of alloimmune sensitization, is associated with the development of pregnancy-related diseases are limited. Numerous reports revealed that the ABO blood group may be associated with some risk factors for unfavorable pregnancy outcomes.  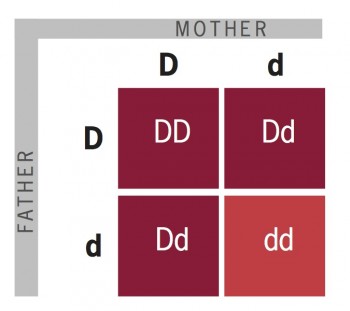
Therefore, several studies showed the clinical significance of the biological characteristics of the ABO blood system, particularly with regard to cancer, cardiovascular disease, and pregnancy-related disease. The blood type may affect human health and diseases with a wide range of expression in human cells and tissues, including platelets, epithelium, and vascular endothelium. The discovery of the Rh blood type has played an important role not only in guiding blood transfusions more scientifically but also in improving experimental diagnoses and clinical immunotherapy. With continuous studies of the Rh blood groups, the Rh blood group system was found to be the most complex system in the RBCs. In 1940, during animal experiments, Landsteiner and other scientists discovered that rhesus monkeys and most human RBCs have antigenic Rh blood types, and this was used in naming the system. 
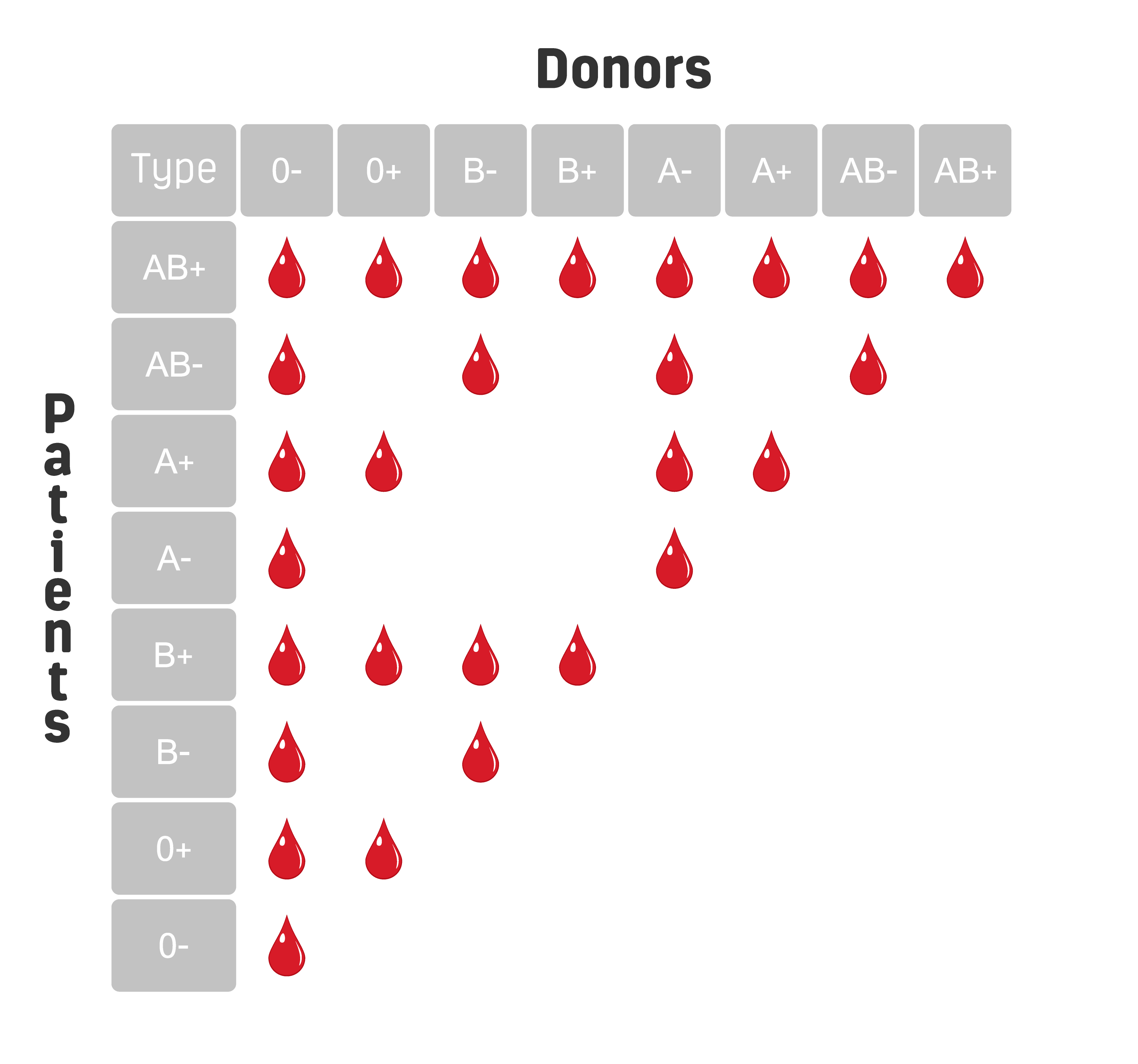
Rh represents the first 2 letters of the name Macacus Rhesus. Based on the presence or absence of the Rh factor, the blood group system is called the Rh blood group system. The ABO blood group system was named according to the different agglutinins, or blood group antigens, including A, B, and H (or O) antigens, on the surface of human RBCs. Karl Landsteiner first discovered the ABO blood group system in 1900 when he was investigating the causes of some fatal transfusions. The 2 main factors that determine the blood type are ABO (A, B, AB, and O) and rhesus (Rh) (positive or negative). Sensitization can also occur if a mother has had a miscarriage, an induced abortion, an ectopic pregnancy, or a blood transfusion.A person’s blood type is determined according to the specific antigen types on the erythrocyte membranes of red blood cells (RBCs). If she becomes pregnant with another Rh-positive fetus, there will be more antibodies that could cause even more serious damage. This condition is called hemolytic disease and can be serious enough to cause illness, brain damage, or even death.Įven after the Rh-positive child is born, the antibodies do not go away. They then become sensitized, causing antibodies to be formed that will fight and break down the fetal blood cells, producing anemia. This can cause a small number of Rh-negative women to react to the fetal blood as if they are allergic to it. Although the mother and fetus do not share blood systems, the fetal blood can go through the placenta into the mother’s system. While carrying this child, the woman may become sensitized. If an Rh-negative woman has a child with an Rh-positive man, their child can be Rh-positive. If this occurs, the negative person will become sensitized, meaning that he or she produces antibodies to fight the Rh factor. The Rh factor causes problems when a person with Rh-negative blood comes in contact with someone with Rh-positive blood.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
